Emergency Dentistry
When a Crown Meets the Gumline, the Details Matter
A crown is supposed to feel like a fresh start. A stronger bite. A tooth you can trust again. But sometimes, after the crown is placed, your gums start sending little signals you did not expect. Soreness that lingers. A bit of bleeding when you floss. A tender spot that seems to flare up at random.
Here’s the good news. Most crown and gum issues are fixable, especially when you catch them early. And often, they are not about the crown being “bad.” They are about the fit, the finish, the gumline environment, and the habits that keep that area calm.
This is the part many people do not hear enough: crowns do not just restore teeth. They also change the neighborhood your gums live in. If the gumline is happy, crowns can last for years and years. If the gumline is irritated, even a beautiful crown can become a constant annoyance.
Below, we’ll walk through what’s normal, what’s not, and what actually helps your gums stay healthy around a crown.
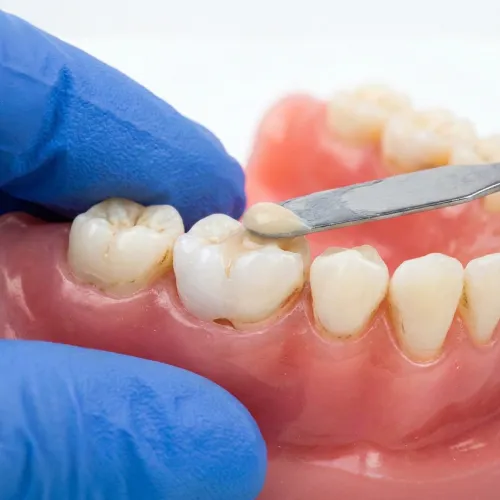
The crown–gum relationship in plain terms
Your gums are protective. They form a seal around your teeth and help keep bacteria from sneaking deeper. When you get a crown, the dentist is essentially rebuilding the tooth’s outer shape, including the area that sits close to the gumline.
That means crown design matters, especially here:
- The edge of the crown (the margin): This is where the crown meets your natural tooth.
- The contour near the gumline: If it is too bulky, gums get inflamed. If it is too thin or poorly adapted, plaque collects.
- The bite and contact points: If the crown hits too hard or traps food, gums can stay irritated.
A well-made crown should feel smooth, easy to clean, and “invisible” to your gums over time.
Common reasons gums get cranky around a crown
Gum irritation around crowns usually falls into a few buckets. Some are short-term and settle down. Others need a quick adjustment.
Here are the most common culprits:
- Healing and inflammation after the procedure. Your gums were moved, retracted, or simply stressed during placement.
- A rough or overhanging margin. Even a tiny ledge can trap plaque like a shelf.
- Cement left behind. A small bit of cement under the gumline can cause ongoing tenderness.
- Crown contour that is too bulky. Gums hate being “pushed” all day.
- Food traps or tight flossing contacts. If floss snaps hard or shreds, that is a clue.
- Bite imbalance. If the crown hits first, the tooth can feel sore and the gums can stay inflamed.
- Gum disease already present. Crowns do not cause gum disease, but they can make existing inflammation more noticeable if cleaning is difficult.
If your gum is sore, bleeding, or puffy around a crown for more than a week or two, that is worth checking. It is usually a small fix, not a major redo.
Why is my gum sore around my crown?
Soreness can mean a few different things, and the details matter. Think about the pattern.
Soreness that is normal early on:
- Tenderness for a few days after placement.
- Mild bleeding when you floss the first week.
- Sensitivity if your gums were inflamed before the crown.
Soreness that should be checked:
- Pain that is sharp, persistent, or worsening.
- Gum swelling that keeps returning in the same spot.
- A pimple-like bump on the gum (possible infection).
- Bleeding every time you brush, even gently.
- Bad taste or odor near that tooth.
Often, the “why” is one of these:
- The margin is irritating the gum.
- There is residual cement under the gumline.
- The crown is too bulky at the gumline, so plaque builds up easily.
- The crown contact is trapping food and you cannot floss properly.
- The bite is high and the tooth is being overloaded.
What you can do at home (short term):
- Brush gently at the gumline with a soft toothbrush.
- Use warm saltwater rinses once or twice daily for a few days.
- Floss daily, slowly, and slide the floss out to the side rather than snapping it up.
- If you use mouthwash, choose an alcohol-free option.
What you should not do:
- Do not stop flossing because it bleeds. That usually makes it worse.
- Do not pick at the gumline with toothpicks or sharp tools.
If the soreness lasts, Prestige Dental can examine the margin, check for trapped cement, and confirm your bite is balanced.
Should there be a gap between my crown and gum?
This is a big one, because people use the word “gap” to describe a few different things.
1) A visible dark line at the gumline:
If you see a thin line where the crown meets the tooth, it could be:
- Natural tooth structure showing.
- Slight gum recession exposing the margin.
- In older crowns, a metal edge may show near the gumline.
A visible line does not always mean the crown is failing, but it can mean the gumline has shifted or the margin needs evaluation.
2) A space that traps food:
If food consistently catches at the crown, that is not something to ignore. Food traps can lead to:
- Gum inflammation
- Bad breath
- Bleeding
- Decay on the tooth under the crown edge
3) A crown margin that is not sealed well:
This is more technical, but important. A crown should have a close, smooth transition at the margin. If the margin is open, bacteria can slip in.
So should there be a gap?
- Your gum should not be permanently “open” around the crown.
- You should not have a consistent food trap or a rough ledge.
- You should be able to floss without shredding or snapping painfully.
If you suspect a real gap, it is worth a professional look. A quick exam can tell whether it is a harmless cosmetic issue, mild gum recession, or something that needs adjusting.
How can I prevent my gums from receding around my crown?
Gum recession around a crown can happen for reasons that have nothing to do with the crown itself, including brushing style, genetics, or inflammation. But crowns do change the cleaning environment, so prevention is all about keeping the gumline calm and plaque-free.
Daily habits that make the biggest difference
Brush like you are polishing, not scrubbing.
- Use a soft-bristled brush.
- Aim the bristles gently toward the gumline.
- Spend extra time around the crowned tooth without pressing hard.
Floss in a crown-friendly way.
- Slide the floss down, hug the tooth, and move gently under the gumline.
- Pull the floss out to the side instead of snapping it back up.
- If floss keeps shredding, that can signal a rough edge that needs smoothing.
Use helpful tools if you have tight spaces or bridges.
- Interdental brushes (the right size matters).
- A water flosser for gumline flushing, especially if gums are sensitive.
- Floss threaders if a crown is part of a bridge.
Protect the gumline from extra stress
If you grind or clench, protect the crown and the gums. Grinding can overload the tooth and irritate the surrounding tissue. A night guard can help prevent micro-movement and inflammation.
Keep up with cleanings. Crowns have margins. Margins attract plaque. Regular professional cleaning helps keep the gumline stable.
Watch for inflammation early. Gums that bleed are usually gums that are inflamed. Treat bleeding as a signal, not a nuisance.
Crown design matters too
Even with perfect home care, a crown that is slightly over-contoured or has a rough margin can keep gums irritated. If your gums keep acting up around a crown, the solution might be as simple as:
- smoothing and polishing an edge
- adjusting the bite
- removing trapped cement
- reshaping the contour near the gumline
Quick self-check: is my crown gum issue minor or urgent?
Book an appointment soon if you notice:
- Bleeding that persists beyond two weeks.
- Gum swelling that comes and goes in the same spot.
- Floss shredding or a constant food trap.
- A crown that feels “high” when you bite.
Call promptly if you notice:
- A pimple-like bump on the gum.
- Facial swelling, fever, or increasing pain.
- Pus, foul taste, or severe throbbing.
Crowns should feel secure, not sensitive
A crown should not leave you constantly wondering if something is wrong. If your gums feel sore, look puffy, or keep bleeding around a crown, you are not being picky. You are paying attention, and that is how you protect your smile long-term.
If you have a crown that doesn’t feel quite right, schedule a visit with Prestige Dental. We can check the gumline, evaluate the crown’s fit and contour, and help you get back to a crown that feels smooth, clean, and comfortable.